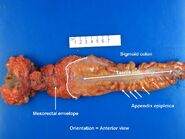
Introduction[]
These are considered complicated specimens, but it all falls back to your basic anatomy and knowing the staging guidelines so that you are able to obtain the information you need. Here are some clues that you may have rectum in your specimen:
- It’s from a colorectal surgeon
- It’s labeled “Sigmoid”. Don’t be fooled – this may have some proximal rectum included
- There’s a history of a rectal tumor
Remember the anatomical differences among the colonic segments:
These rectal resections can be done either as a primary treatment of after a first round of chemotherapy and/or radiotherapy. The most common types of surgeries include:
- Low anterior resection = for cancers in proximal 2/3rds of the rectum
- Abdominoperineal resection = distal rectum + anal canal + perianal skin = for tumors of the distal 1/3rd of the rectum.
Note that the "radial margins" will be different depending on where you are in the rectum.
Fresh Handling[]
- Measure: length and greatest diameter, staple lines if any, mesorectal fat, mass if it’s palpable from the outside.
- Orient the specimen: the peritoneal lining (shiny, smooth and glistening) falls more inferior in the anterior aspect, and more superior in the posterior aspect. The posterior/inferior aspect is dominated by the mesorectal envelope, which is more ragged and irregular.
- Photograph the specimen before inking, from the anterior and posterior aspects
- Important step unique to rectum specimens: Evaluate the excision of the mesorectum (mesorectal envelope):
- Complete: Good bulk, smooth, no surface defects > 5mm depth, no distal “coning”
- Nearly complete: Moderate bulk, surface defects > 5mm depth but not to M. propria
- Incomplete: Little bulk, surface defects to M. propria
- Describe mesorectum excision as complete, nearly complete, or incomplete based on the specified criteria – STATE YOUR CRITERIA in your report – DO NOT TAKE THIS LIGHTLY! It’s a statement as to the adequacy of surgical technique with direct prognostic significance.
- Ink: use different colors to designate the anterior and posterior mesorectal envelope (e.g. anterior blue, posterior green); then ink the peritoneal surface with a third color (e.g. black). The only true radial margins will be the mesorectal envelope and the root of the mesentery, NOT the peritoneal lining.
- Open up the specimen longitudinally trying not to cut through the tumor, and gently remove blood, stool or necrotic debris with a saline rinse.
- Photograph the opened specimen and use it as a guide or diagram for your sectioning.
- Pin on corkboard and fix overnight.
Grossing In[]
- Identify the type of resection: abdominoperineal resection (APR), low anterior resection, rectosigmoidectomy…
- Describe measurements as above. Correctly identify what is sigmoid and what is rectum – measure from rectosigmoid junction.
- Describe the tumor characteristics if there is a mass:
- Tumor size
- Shape (fungating, polypoid, flat)
- Surface (ulcerated, necrotic)
- Color
- Location: distance from dentate line, state tumor is located “in the rectum”, or “at the anorectal junction”, etc.)
- Distance from proximal and distal margins of resection
- If prior chemo-radiation has been given, there may not be an identifiable mass. In this case, describe the area of induration (feeling works better than sight in this case!) and/or ulceration.
- At this point, serially section the tumor (or area of induration) full thickness, into approximately 5 mm thick sections, transverse to the longitudinal axis of the specimen, and keeping orientation (i.e. from proximal to distal or viceversa). Lay the sections on a cutting board and take photographs. Here is an example:
- Measure distance from lesion to mesorectal radial margin – photograph relevant slice on closer view. This will be the most relevant radial margin, which predicts local recurrence and survival. The only one to document this is you, the grossing resident!!
- Summary of sections:
- Sections of tumor (3), including junction of carcinoma with normal mucosa on at least one, and full depth (with inked margin), including serosa on at least two sections.
- If specimen is obtained after treatment and tumor is not grossly evident, then submit the entire area of fibrosis/induration/ulceration. A complete pathologic response (no residual tumor on pathologic examination) is seen in 10% to 30% of patients, so the entire area needs to be submitted to find microscopic residual disease.
- Other lesions, if any.
- One section of uninvolved mucosa
- Margins of resection, proximal and distal. A shave margin may work for the proximal margin. For abdominoperineal resections, the distal margin will be a relatively large amount of skin. Take a longitudinal section of the tumor towards the margin, if possible.
- Lymph nodes: remember you must get at least 12. Measure the enlarged lymph nodes and note if they seem involved by tumor. If so, a representative section is sufficient. Submit all other nodes entirely.
Sample Dictation[]
The case is received in one formalin-filled container, labeled with the patient's name and medical record number, and designated "rectum and sigmoid colon". It consists of an abdomino perineal resection specimen measuring 40 cm in length. The specimen consists of sigmoid, rectum and perianal skin; the sigmoid portion measures 31 x 9 x 4 cm; the rectum measures 13 x 9 x 7 cm; and the skin measures 9 x 6 cm and shows a protruding mass measuring 1.5 x 1.0 x 0.5 cm. There is no tumor identifiable on the surface of the skin. The sigmoid colon is covered by mesenteric fat and peritoneum and the rectum is covered by mesorectum both anterior and posteriorly. On the posterior aspect there is a potential perforation identified at the level of the tumor, which after discussion with the surgeon is designated as a "surgical disruption" and not true tumor perforation. The specimen is inked as follows: Proximal margin is red, radial mesenteric margin is black, anterior mesorectum is blue, posterior mesorectum is green. The proximal staple line measures 3.0 cm, it is removed and the shaved margin is submitted as 1A. The specimen is opened from the anterior aspect to reveal an ulcerated necrotic mass measuring 10.0 x 9.0 cm involving the rectum, the dentate line and the anal canal, and located 3.5 cm from the skin margin. The colonic mucosa appears diffusely dark and erythematous, but no mucosal lesions are identified. Focally it appears thinned with an average thickness of 0.4 cm. A representative section of the colonic mucosa is submitted in 1B. Sectioning through the tumor in relation to the perianal skin margin is submitted in 1C. The rectum containing the tumor is then serially sectioned from distal to proximal to reveal that the maximum thickness of the tumor is approximately 1.2 cm and that the ulcerated area of tumor appears to infiltrate through the muscularis propria into the subserosa and underlying fat. The posterior mesorectum is incomplete, with areas that approach the muscularis propria. Representative sections of the tumor are submitted as 1D - 1HH. 1II contains a section of rectal mucosa adjacent to the tumor. Potential perirectal lymph nodes submitted as 1JJ - 1NN, and additional pericolonic potential lymph nodes submitted as 1OO - 1QQ.
Review and Signout[]
As mentioned, you need to document the presence or absence of residual tumor if it has been treated. Describe the histology, the grade of differentiation, and mention all the features needed for staging: depth of invasion, lymph node involvement, etc. Don't forget the importance of the radial margins!
Sample diagnostic lines[]
- Rectum and sigmoid colon, abdomino-perineal resection:
- A. Rectal adenocarcinoma, (well, moderately, poorly) differentiated, x cm, invading (into submucosa, into but not through the muscularis propria, through the muscularis propria into the perirectal soft tissue), with (mucosal ulceration and superficial necrosis), (focally approaching, present at, negative) the posterior inked radial margin of resection, see note.
- B. X lymph nodes, negative for metastatic carcinoma (0/X). OR Metastatic carcinoma in X of Y lymph nodes (X/Y).
- C. Proximal colonic and distal perianal skin margins of resection free of tumor.
- Rectum and sigmoid colon, abdomino-perineal resection:
- A. Rectum with mucosal ulceration and fibrosis, consistent with treatment effect, no evidence of residual carcinoma seen.
- B. Proximal and distal margins of resection free of tumor
- C. X lymph nodes, negative for metastatic carcinoma (0/X).
- Rectum and sigmoid colon, abdomino-perineal resection:
A. Residual rectal adenocarcinoma, multiple microscopic foci, involving (submucosa, into but not through the muscularis propria, through the muscularis propria into the perirectal soft tissue), with (associated treatment effect), (focally approaching, present at, negative) the posterior inked radial margin of resection, see note. B. Proximal and distal margins of resection free of tumor C. X lymph nodes, negative for metastatic carcinoma (0/X).
Return to Gastrointestinal Grossing